Rural Hospital Closures: How COVID-19 Impacted Hospitals
Tables of Contents
Hospitals and other healthcare facilities are critical to the American population — and the economy.
In 2018, U.S. hospitals and health systems provided emergency care to 143 million people, performed more than 28 million surgeries, and delivered nearly 4 million babies, according to the American Hospital Association (AHA). The Centers for Medicare and Medicaid Services (CMS) reports that in the same year, healthcare represented about 18% of the U.S. economy.
However, a spate of hospital closures, exacerbated by COVID-19, is leaving too many people without convenient access to healthcare and too many communities without an important economic driver. Rural communities — which account for 46 million people, according to the Centers for Disease Control and Prevention (CDC) — are bearing the brunt of this healthcare trend.
The result: new concerns about rural hospital closures.
Hospital Closures Across the U.S. from COVID-19
Hospital numbers were already declining as the U.S. approached the heart of the COVID-19 pandemic in 2020. In 2019, the U.S. had 6,090 hospitals, 56 fewer than the previous year, according to the AHA. Similarly, 2018 saw 64 fewer hospitals than the year before.
When COVID-19 hit, this already-concerning situation became dire. Bloomberg reported that more than three dozen U.S. hospitals had already gone bankrupt by the fall of 2020. At least 30 hospitals met the same fate in 2019.
The increase in hospital closures was especially profound in rural communities, with a city manager in Bowie, Texas, telling Bloomberg that rural hospitals were “closing right and left” in 2020.
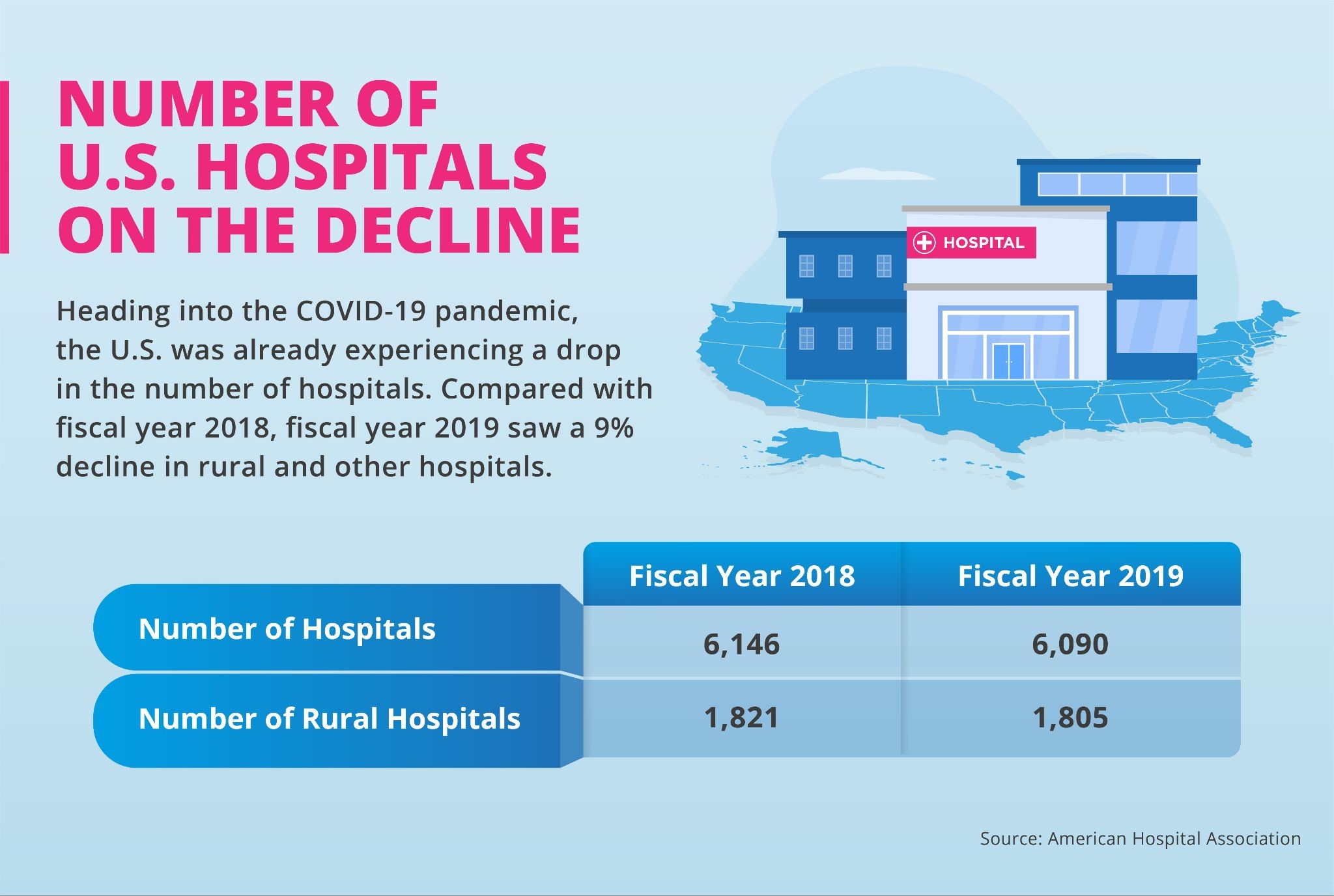
Heading into the COVID-19 pandemic, the U.S. was already experiencing a drop in the number of hospitals, according to American Hospital Association data. Compared with fiscal year 2018, fiscal year 2019 saw a 9% decline in rural and other hospitals. The number of hospitals in fiscal year 2018 was 6,146, compared to 6,090 in 2019. The number of rural hospitals in fiscal year 2018 was 1,821, compared to 1,805 in 2019.
COVID-19’s effects on hospitals may not end with the pandemic. A 2021 Kaufman Hall study showed that the pandemic could lead hospitals to losses of between $53 billion and $122 billion during the year, depending on how the pandemic progresses.
Challenges Facing U.S. Hospitals
Changes in insurance and patient demographics are among the reasons hospital closures have been a concern in recent years, both before and during the pandemic. Following is a look at some of the forces at work in these closures.
Hospital Consolidations
Hospital mergers and acquisitions over the past two decades have created large hospital systems that often cater to well-insured patients. These hospitals, often located in urban areas, can charge higher prices, even as smaller hospitals struggle to cover rising expenses.
Changing Demographics
Demographic shifts have been placing greater demands on hospitals in recent years. The world’s population is getting older, placing additional stress on hospitals as they care for chronic conditions. Additionally, Brookings reported in 2018 that half the world’s population could be defined as middle class or wealthier — and individuals with this socioeconomic status enjoy comforts that can promote a more sedentary, unhealthy lifestyle.
Outpatient Care Focus
Deloitte reports that the healthcare industry has shifted toward more virtual care and fewer hospital beds. This trend has left medical providers to focus on other ways to stay financially solvent, with less emphasis on in-hospital patient care and more emphasis on outpatient services. Elective procedures and outpatient visits often provide the highest profit margins, but COVID-19 restrictions forced hospitals to curtail many of these offerings during the pandemic.
Medicaid Coverage Gaps
In July 2021, the Kaiser Family Foundation reported that 12 states had not expanded Medicaid coverage as permitted under former President Barack Obama’s healthcare law: the Affordable Care Act (ACA). The ACA expands Medicaid coverage for most low-income adults, but states can opt out of this additional coverage. In states that choose not to adopt this expansion, low-income individuals face the prospect of a gap in insurance coverage to receive healthcare — including that provided by hospitals, which in turn receive less reimbursement.
What Is a Rural Hospital?
As hospitals in general grapple with the financial implications of COVID-19 and other challenges, rural hospitals are feeling the effects even more acutely. Rural hospital closures are affecting an increasing number of communities.
What is a rural hospital, exactly?
Defined broadly, a rural hospital is located outside a metropolitan area. Because rural hospitals are often the only sources of healthcare in a community, they tend to provide more services than urban hospitals do. Rural hospitals often provide a continuum of care, from primary care to long-term medical assistance, and are often among the top employers in the community.
What Defines Rural?
Different U.S. government entities — including the U.S. Census Bureau, the Office of Management and Budget (OMB), and the Federal Office of Rural Health Policy (FORHP) — have different guidelines for defining rural populations.
The federal government has two main sets of criteria for what defines rural: those from the U.S. Census Bureau and the OMB. The FORHP considers elements from both agencies’ definitions when determining eligibility for federally funded services for rural healthcare.
U.S. Census Bureau Definition of Rural
The U.S. Census Bureau doesn’t specifically define rural areas, but rather considers areas that don’t fall under its definition of urban to be rural populations. The U.S. Census Bureau defines urban clusters as those of at least 2,500 people.
Office of Management and Budget Definition of Rural
The OMB also classifies counties according to population, and it considers any county not classified as part of a metropolitan area to be rural. The OMB considers metropolitan areas to be those with a population of 50,000 or more people in a core urban area.
Federal Office of Rural Health Policy Definition of Rural
The FORHP classifies all nonmetropolitan counties as rural. To evaluate whether a rural community is eligible for federal programs, the FORHP also considers other census-based criteria, such as those determining rural-urban commutes. The Health Resources & Services Administration (HRSA) offers a tool to determine whether a county is rural under FORHP guidelines.
Categories of Rural Hospitals
The Rural Health Information Hub (RHIhub) provides information about the hospital designations and provider types from the Centers for Medicare & Medicaid Services (CMS). The following CMS designations give certain providers special consideration for federal insurance reimbursement:
- Critical access hospital. A CAH houses no more than 25 acute care beds and is located more than 35 miles (or 15 miles of mountainous terrain or roads) from the nearest hospital.
- Rural referral center. An RRC receives referrals from a nearby rural acute care hospital.
- Sole community hospital. A SCH meets distance criteria indicating the facility is the only hospital of its kind serving a community. Distance requirements vary according to the hospital’s rural status and how accessible it is (based on factors such as terrain and weather).
- Low-volume hospital. A LVH is a facility with fewer than 3,800 patient discharges in the previous year that is located more than 15 miles from the nearest acute care hospital.
- Medicare-dependent hospital. An MDH contains 100 or fewer beds, and at least 60% of its patient population is insured by Medicare.
COVID-19 is the latest in a host of challenges facing rural hospitals in the U.S. Other challenges include the following, according to the American Hospital Association: insurance coverage, patient demographics, geographic isolation, employee recruitment, aging facilities, outpatient care emphasis, mental healthcare needs, regulatory burdens, prescription costs, the opioid crisis, and cyber threats.
Why Are Rural Hospitals Closing?
Today’s healthcare environment provides challenges that are leading to rural hospital closures. In 2020, the Center for Healthcare Quality and Payment Reform (CHQPR) reported that 800 rural hospitals nationwide were at risk of closure. Why are rural hospitals closing?
Issues Facing Rural Hospitals
According to the AHA, one challenge facing rural hospitals is that their patients are often “older, sicker, and poorer” than national averages, putting greater demands on the healthcare system. That makes rural hospital closures even more concerning. Following are some of the additional issues that play a role in why rural hospitals are closing.
Low Reimbursement Rates
Rural hospitals are often more dependent on payment from government insurance programs, such as Medicaid and Medicare, whose historically low reimbursement rates can make it difficult for hospitals to meet expenses. They also serve a high number of patients left behind in the shift from a manufacturing economy, leaving these patients either uninsured or underinsured and unable to pay for emergency and other acute care services.
Reduced Patient Volume
Rural populations are declining, down by nearly a million people between 2016 and 2019, according to Macrotrends. This shift leaves hospitals in these rural areas with fewer patients to access their services, even as the increased healthcare needs of rural Americans and the aging U.S. population leave people in greater need of care.
Increased Regulation
The lower patient volume of rural hospitals means that their per-patient cost of compliance is higher than that of other hospitals. Adhering to regulatory requirements also requires a level of staffing that many rural hospitals struggle to meet.
Rural Patient Demographics
Obesity, diabetes, hypertension, and smoking rates are higher in rural areas, according to a report from PBS. Additionally, the CDC reports that residents in rural areas are more likely to die from the following conditions:
- Cancer
- Chronic lower respiratory disease
- Heart disease
- Stroke
- Unintentional injury
The PBS report also noted that 95% of rural counties had 100 or more COVID-19 cases per 100,000 residents from August 2020 to February 2021, meeting the criteria for being a COVID-19 “red zone” that the White House coronavirus task force has put forth. Meanwhile, the report indicated that many residents who rural hospitals serve lack trust in the medical system.
Rural Hospitals and COVID-19 Costs
Rural hospitals already at risk of closing had few financial reserves to accommodate the demands of the coronavirus. They were left scrambling to cover lost revenue from delayed elective procedures, pay for personal protective equipment (PPE), and compensate for a job loss-related drop in access to health insurance among their patients.
Rural Hospital Closings and Community Impact
Hospital closures can be devastating to rural communities. Following are some of the effects that rural hospital closures may have on communities.
Fewer Options for Care
Rural hospital closures often leave an area with little to no nearby options for healthcare. A 2021 report from the U.S. Government Accountability Office (GAO) showed that when rural hospitals closed from 2013 to 2020, people living in nearby areas had to travel about 20 miles farther for common services, including inpatient care. For less common services, such as alcohol or drug abuse treatment, residents had to travel 40 miles farther.
Dangers to Health
The lack of local care can have serious consequences for rural residents, particularly in cases that call for quick access to treatment. Pregnant women and their babies are among those at risk; in 2018, a report in JAMA showed an increase in preterm births in rural areas where the obstetrics units of hospitals had closed.
Increase in Mortality Rates
Lack of accessible care in rural areas also leads to higher mortality rates, according to the National Bureau of Economic Research (NBER). The NBER found that rural hospital closures resulted in a mortality rate increase of 6% to 9%.
Loss of Tax Revenue
Communities also feel the impact of rural hospital closings in ways that go beyond health. The local economy can take a hit as well, with closures leaving the local tax base in distress, the community with fewer highly educated professionals, and local schools with a declining number of students. High-quality hospitals can also attract other top companies to an area, and communities lose that asset when hospitals close.
U.S. Hospitals: Closing Statistics
Hospitals’ closing statistics paint a troubling picture: The AHA reports 9% annual declines in the number of rural and other hospitals. The CHQPR indicates that 800 rural hospitals were at risk of closure based on persistent losses and low funding reserves as of May 2021: 500 (more than a quarter of rural hospitals in the nation) at immediate risk and 300 more at risk in the near future.
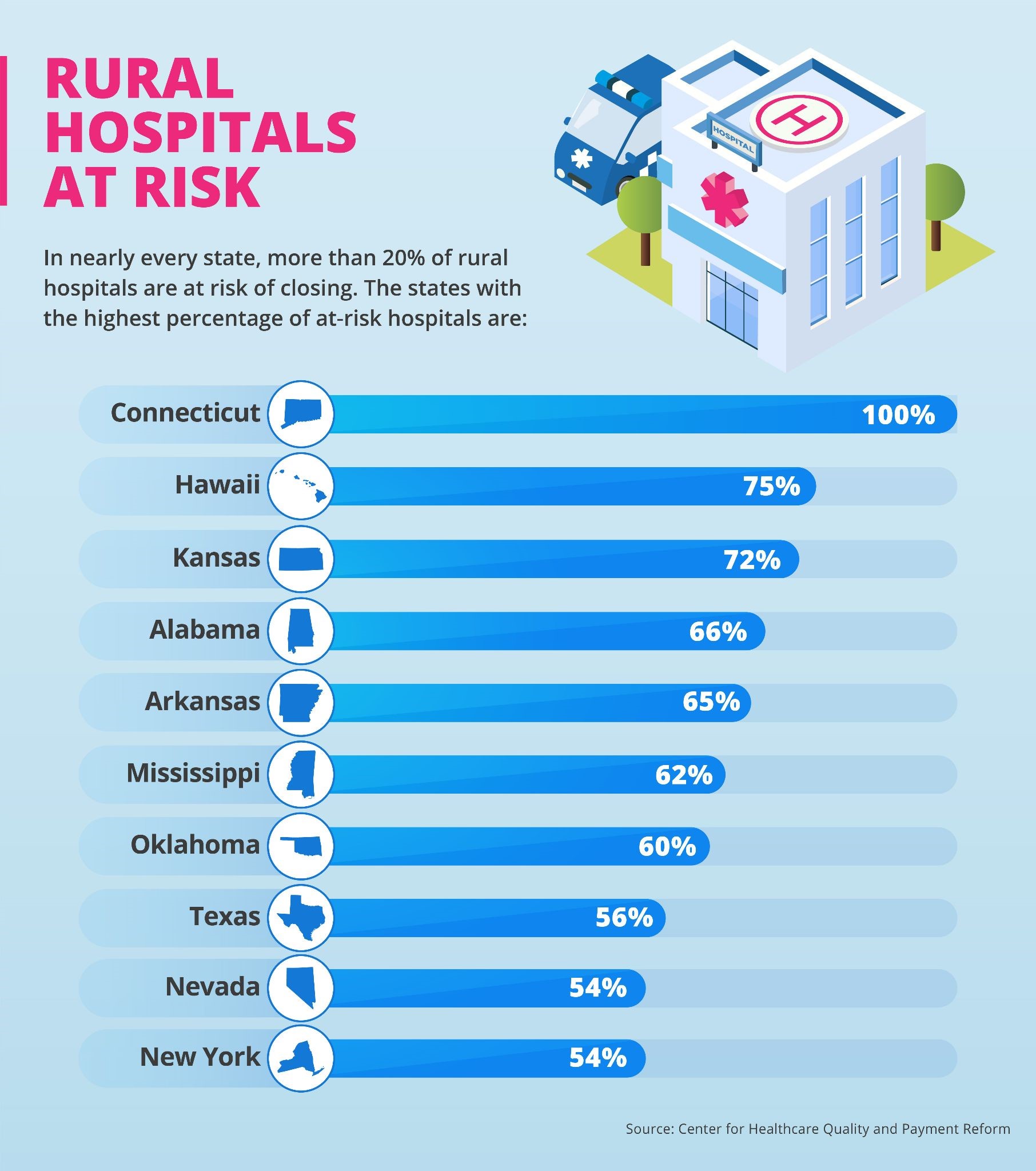
In nearly every state, more than 20% of rural hospitals are at risk of closing, according to the Center for Healthcare Quality and Payment Reform. The states with the highest percentage of at-risk hospitals are: Connecticut, 100%; Hawaii, 75%; Kansas, 72%; Alabama, 66%; Arkansas, 65%; Mississippi, 62%; Oklahoma, 60%; Texas, 56%; Nevada, 54%; and New York, 54%.
Those hospital closings statistics seem even more daunting considering the nation already struggles with healthcare access. In the 2019 Global Health Security Index, the U.S. was ranked No. 175 out of 195 countries for access to care. In 2020, the Peterson-KFF Health System Tracker ranked the U.S. below many similarly wealthy nations in the number of hospital beds per capita, with 2.8 hospital beds for every 1,000 people. Austria, for example, had 5.2 hospital beds per capita, and Switzerland and Germany each had 4.3.
What Rural Small Town Hospitals Can Do to Survive
Faced with multiple obstacles and a challenging outlook, what can rural small town hospitals do to survive? From implementing debt management measures to building customer loyalty, rural hospitals are taking steps to stave off closure and continue providing valuable services. Following are some of the measures that rural small town hospitals and hospital organizations are taking.
Bolstering Residency Programs
A 2019 report in Family Medicine showed that medical residents who train in rural areas are two to three times more likely to remain in rural small-town areas to practice. Hospitals are increasing their number of residents to enhance their staffing and increase the availability of healthcare.
Self-Assessment
To gauge where they can improve, rural hospitals are conducting thorough reviews of their finances. These reviews check for issues such as outdated systems and billing issues.
Encouraging Policy Changes
To address policy issues that can cut rural hospitals’ profits, hospitals and organizations that represent them are working to encourage changes at the federal level. They’re providing input on issues such as Medicare reimbursements, regulatory burdens, telehealth coverage, and prescription costs.
Identifying New Revenue
Rural hospitals are seeking new ways to generate revenue. They’re working with outpatient healthcare providers, for example, to offer programs such as mental health services and entering into revenue-sharing agreements.
Managing Debt
Rural hospitals are looking for ways to handle their debt. The options include working with debtors and exploring refinancing options.
Offering Telehealth Services
To enhance access to care in remote areas and accommodate health concerns related to COVID-19, rural hospitals are increasing their remote care offerings. In addition to online appointments, hospitals are offering web-based options for prescription services.
Strengthening Customer Loyalty
To capitalize on consumer desire to support local businesses, rural hospitals are working to promote their services in their communities. From sponsoring events to enhancing online services, they’re making efforts to become more visible.
Resources for Assistance with Rural Hospital Challenges
Rural hospitals can turn to online resources for assistance with challenges in areas such as billing, quality of care, technology needs, and COVID-19 response. Following are some of those resources.
- The CMS Rural Health Resources link to CMS materials related to COVID-19, payment and billing, and chronic care.
- The HRSA Rural Health Resource Guide connects healthcare professionals with opportunities to collaborate, learn about best practices, and access research related to rural healthcare.
- The National Rural Health Resource Center presents webinars, group discussions, podcasts, and other materials designed to help healthcare providers in rural communities enhance their work.
- The RHIhub provides links to funding, billing, and treatment resources related to COVID-19 and various other healthcare topics to help executives, managers, and providers at hospitals and other inpatient facilities maintain services.
- The Office of the National Coordinator for Health Information Technology (ONC) Resources for Critical Access Hospitals and Small Rural Hospitals offer guides to assist with implementing technology, including electronic health records (EHRs) and telehealth, to support and expand access to rural healthcare.
Rural Hospitals: A Vital Healthcare Provider Working to Overcome COVID-19 Challenges
Rural hospitals are valuable assets to the health of their economies, but years of challenges to U.S. hospitals, worsened by the COVID-19 pandemic, have left the nation with a decreasing number of hospitals and a growing number of rural hospital closures. Through steps to save hospitals and find cost-efficient methods for providing care, hospitals are working to ensure that all Americans have access to the local care that will improve rural health and economic conditions.
Infographic Sources
American Hospital Association, Fast Facts on U.S. Hospitals, 2020
American Hospital Association, Fast Facts on U.S. Hospitals, 2021
Center for Healthcare Quality and Payment Reform, “Rural Hospitals at Risk of Closing”

